The Biomechanical Bridge: Connecting Hip Mobility to Low Back Health
Written by Charlie Annunziata, DC
Low back pain (LBP) is the second most common symptom-related reason for clinician visits in the United States (skin disorders was number one) and is THE most common indication for Chiropractic care. In fact, up to 84% of the US population has been found to report LBP symptoms at some point during their lifetime. However, the etiology of LBP is not well understood considering the evidence that people without LBP have structural changes and many LBP patients have no structural changes on imaging studies of the lumbar spine. Long and colleagues performed a standardized mechanical assessment on 312 patients with LBP, with and without sciatica. They were able to successfully subgroup 230 (74%) of these patients, however 26% of the patients did not fit into a subgroup (Long A, 2004). So, the question remains: how do health care providers best assess people with LBP in order to develop a specific and successful treatment recommendation? Might we look beyond the spinal column for the source of, or contributor to, pain and loss of function?
Research now shows that limited hip internal rotation can significantly contribute to low back pain. This may be caused by hip joint variants but more commonly by trauma causing adhesion of the hip joint capsule or even prolonged sitting which over activates the hip flexors and abductors and under activates the hip extensors and adductors. This article explores the relationship between hip mobility and lower back health, highlighting how restricted hip internal rotation can lead to various issues in the lumbar spine.
Biomechanics
Hip internal rotation plays a crucial role in normal gait, balance, and functional movement. When this range of motion becomes restricted, it forces compensation in other parts of the body, particularly the lumbar spine (Sadhegisani, 2015). This compensation can lead to several problems:
Lumbar Over-rotation: Reduced hip mobility causes the lumbar spine to over-rotate during everyday movements, increasing pressure on intervertebral discs, muscles, and ligaments.
Pelvic Dysfunction: Limited internal rotation, especially when asymmetrical, can cause pelvic imbalances that pull the lower spine into abnormal positions.
Altered Biomechanics: The lack of hip internal rotation changes overall movement patterns, altering the natural biomechanics of the spine and pelvis.
What Does the Research Say?
The correlation between limited hip internal rotation and low back pain is elucidated in many recent studies. Sadhegisani reported that asymmetrical and limited hip internal rotation ROM were common findings in patients with LBP. Reduced and asymmetrical total hip rotation was also observed in patients with LBP. However, none of the studies explicitly reported limited hip external rotation ROM. Proving that not all hip rotation ROM affects low back pain, just internal rotation.
Ellison et al. reported that deficits in hip internal rotation are related to both LBP and sacroiliac joint pain (JB, 1990). Another study found that patients with low back pain and positive hip findings such as a positive anterior hip impingement test, FABER test, and/or log-roll test, have more pain and worse function compared to those without positive hip findings. Research has also demonstrated that a loss of hip internal rotation can prevent the pelvis from rotating properly over the stance limb during gait, affecting the coupling mechanics of the sacrum and lumbar spine (Yoon, 2024).
What Causes Hip-related Low Back Pain?
The development of low back pain due to limited hip internal rotation can occur through several mechanisms such as compensatory spinal motion, pelvic and lumbar muscle imbalances, and repetitive stress syndrome (Sadhegisani, 2015). When hip rotation is limited, the spine may compensate by rotating, extending, or flexing more than it should. Restricted hip mobility can lead to muscle imbalances through overactivity and tightness related muscles such as the piriformis, potentially compressing the sciatic nerve. Repetitive stress injuries also come into play. Even small amounts of repeated rotation in the spine, compensating for lack of hip mobility, can produce microscopic injuries to spinal structures over time.
How to Make the Diagnosis
Limitations in hip internal rotation can be diagnosed through several assessments such as:
Seated Test: The patient sits on the edge of a treatment table with feet dangling, knees and hips flexed to 90 degrees. They are asked to keep their knees together while moving their ankles apart. The Chiropractor may apply overpressure to add a passive component.
Prone Test: With knees together and flexed to 90 degrees, the ankles are allowed to fall apart. Overpressure can be applied for a passive component.
Gait Observation: While assessing gait you may notice movement compensations such as overpronation of feet, knee valgus, reduced step length, external rotation of the foot during stance phase, increased lumbar and knee extension.

How to Correct
To correct limited hip rotation, it is best to use a combination of hip joint mobilization, stretches, and strengthening exercises. Joint play assessment with mobilization in the direction of limited movement through manipulation and hip scouring techniques as well as soft tissue mobilization to the ipsilateral psoas, glute medius and piriformis muscles are a great place to start. Followed by hip stretching and strengthening exercises such as:
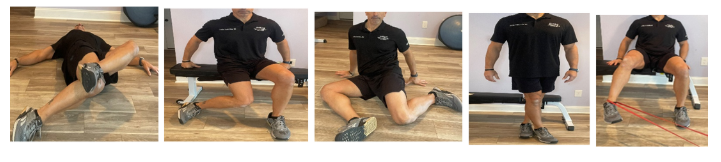
Twisted Legs Hip Internal Rotation: Sit on the ground, let both knees fall to one side, and place the top foot on the opposite knee.
Seated Hip Internal Rotation: Sit with knees at 90 degrees, flex one foot, and turn the inner thigh toward the ground. Perform 20-30 reps per side.
90/90 Hip IR Lift Offs: In a 90/90 position, lift the back leg while focusing on internal rotation.
Step Across: In a staggered stance, step across the midline with the back foot while keeping the front leg still. Repeat 20 times.
Band Lateral Distraction IR Rockbacks: Seated patient uses a band for lateral distraction while rocking and maintaining internal rotation of the hip against resistance, focusing on keeping a flat back.
Swivel Chair (not pictured): This is a great stretch your patients can do right in their office. Place your knee on a swivel chair and swing your foot outward, keeping the pelvis still. Repeat 20 times.
By incorporating hip internal rotation assessment into their evaluations, chiropractors can develop more effective and comprehensive treatment strategies that address both spinal and hip dysfunction as a cause of low back pain, leading to improved patient outcomes and long-lasting relief.
References
JB, E. (1990). Patterns of Hip Rotation ROM: A Comparison Between Healthy Subjects and Patients with LBP. Physiological Therapeutics.
Long A, D. R. (2004). Does It Matter Which Exercise? A Randomized Control Trial of Exercise for Low Back Pain. Spine.
Sadhegisani, M. (2015). Correlation Between Hip ROM Impairment and Low Back Pain: A Literature Review. Ortop Traumatol Rehabil.
Yoon, J.-y. (2024). Impacts of Asymmetric Hip Rotation Angle on Gait Biomechanics in Patients with Knee Osteoarthritis. Knee Surg Relat Res.
Charles Annunziata DC, CFMP graduated from Life University in 1998 and has been in full-time practice ever since. Dr. Annunziata is certified in Functional Medicine and is a nationally recognized lecturer on Chiropractic though both in-person and on-demand seminars available at procreditsce.com. For any questions, please feel free to contact Dr. Annunziata at drcharlie@procredits.com.