The Most Common Conditions Chiropractors Treat: NHIS Insights
NHIS data reveals why millions choose chiropractic care. Discover the most common conditions chiropractors treat — from back and neck pain to headaches and arthritis.
A 2017 study analyzing NHIS data found that back pain (63%) and neck pain (30%) are the most common reasons adults seek chiropractic care. At Thrive Sports & Spine, these are among the top conditions we treat daily.
Back Pain: The #1 Condition
Back pain remains the leading driver of chiropractic visits. Whether acute (lifting injury) or chronic (degenerative disc disease), chiropractic adjustments and rehabilitation provide natural relief.
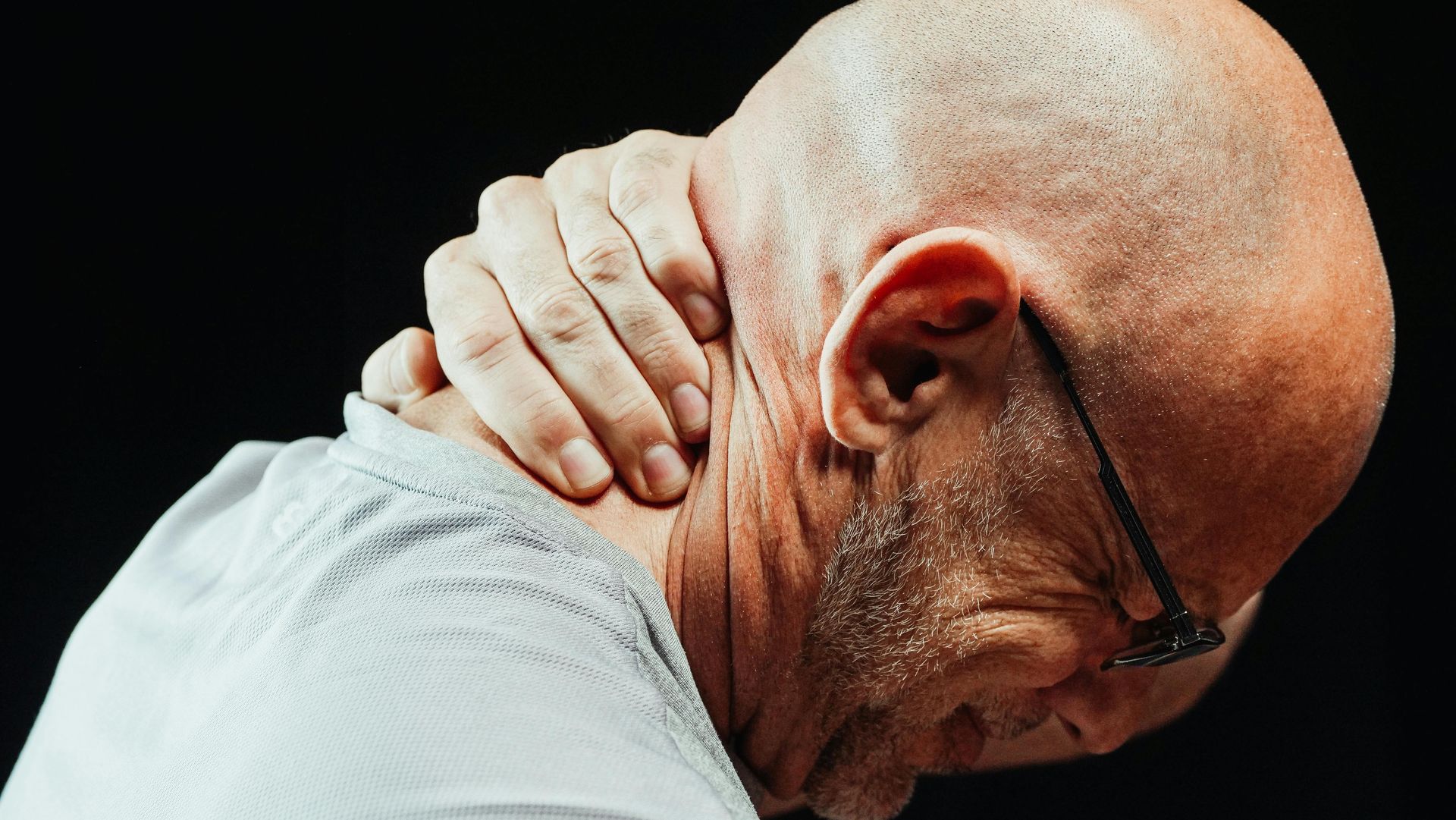
Neck Pain: Posture, Tech, and Injury
Modern lifestyles increase neck stress from phones, computers, and stress. Chiropractic restores normal motion, decreases pain, and reduces muscle tightness.
Headaches & Migraines
Cervical spine dysfunction often contributes to tension headaches. Chiropractic helps reduce frequency and intensity, especially when combined with posture correction.
Arthritis & Stiff Joints
Older adults commonly seek chiropractic for stiffness and joint pain. Gentle mobilization helps preserve function and delay progression.
Integrated Care Matters
About 63.8% of patients in the NHIS study reported that combining chiropractic with conventional medicine was helpful — reinforcing that chiropractic plays an important role in integrative care.
Conclusion:
If you’re experiencing back pain, neck pain, headaches, or arthritis, you’re not alone — these are the most common reasons patients turn to chiropractic care. Thrive Sports & Spine specializes in treating these conditions with evidence-based, patient-centered care.
Reference:
Adams J., et al. “The Prevalence, Patterns, and Predictors of Chiropractic Use Among US Adults: Results From the 2012 NHIS.” Spine 2017;42(23):1810-1816.
Beyond the Adjustment: How Your Home Habits Amplify Chiropractic Care
At our chiropractic office, we talk a lot about spinal alignment, joint mobility, nervous-system health and how we can help you feel better, move better and live better. What many people don’t realize is that the magic really happens outside the clinic, too — your home habits, movement, posture and recovery all amplify (or undermine) what we do in our sessions.
A recent article published in IJSNEM underscores an important principle: recovery, adaptation and musculoskeletal resilience don’t occur simply by the passive act of treatment, but through the ongoing interplay of mechanical stimulus, recovery behaviors and nutritional/functional support. Although the study focuses on exercise-nutrition interactions, the broader lesson carries over to chiropractic care: what happens after your adjustment matters.
Why Home Behavior Matters
- Mechanics still count
When we perform an adjustment, mobilize a joint, release tension in soft tissue or correct posture, we are giving your body a “reset” or a signal: you can move differently now. But if you immediately return to poor posture, repetitive strain or inefficient movement patterns, you reduce or undo the benefit we just instilled. - Recovery isn’t just sleep
The IJSNEM-type study shows that nutrients, movement timing and recovery habits influence the tissue-adaptation process. In our world, that translates to more than sleeping well, it means micro-movements, posture breaks, hydration, gentle mobility work and giving your body cues that “yes, we’re moving well now”. Your home routine is your recovery routine. - Consistency trumps singular sessions
One great visit helps. Six great visits help more. But without accompanying home behaviour, the rate of change slows. The research literature in sports science is full of examples where “the exercise + nutrition” combo matters far more than either alone. Similarly, the “adjustment + home habit” combo is what drives the best outcomes.
What You Can Do At Home
Here are five practical ways to extend your chiropractic care into your daily life:
- Micro-mobility breaks: Every hour, stand up and take 30 seconds to do a gentle spinal twist, shoulder roll or hip hinge. This interrupts prolonged postures and keeps your nervous system responsive.
- Posture awareness: At your computer, phone or while driving, check your alignment. Are your ears over your shoulders? Shoulders over hips? If not, correct it and hold 10-15 seconds.
- Soft-tissue self-care: Use a foam roller, lacrosse ball or simple stretching routine (we’ll show you what works). This supports tissue quality and helps joints move more freely between visits.
- Hydration + nutrition: Adequate water, good protein, plenty of fresh produce = supporting tissue healing, joint lubrication and nervous-system resilience. While the IJSNEM article focused on exercise nutrition, this principle applies universally.
- Quality sleep + nervous system reset: Sleep is when the body heals, re-organizes and rebuilds. Make your environment calm, screens off at a reasonable hour, and consider 5 minutes of diaphragmatic breathing before bed to down-regulate your nervous system.
How We Integrate This Into Your Care
In each visit, we will not only adjust and mobilize, we will also coach you on what to do at home until your next session. We’ll assess your movement patterns, posture, daily habits and design a simple “home plan” that fits your lifestyle. Because true change happens when clinic meets home.
Final Thoughts
Think of our work together as planting a seed. The adjustment is the planting; your home habits are the water, sunlight and soil. Without both, the growth is limited. The IJSNEM-type research reminds us that optimisation is a combination of professional input + personal discipline. We’re here for the professional input. You’re here for the personal discipline. Together, we make the difference.
If you’re ready to take your home habits to the next level and get the most out of your chiropractic visits, ask us about your personalised at-home plan at your next session!
Reference:
Mala, J., Blazek, Z., Maly, T., & Zahalka, F. (2024). Effect of nutrient timing on muscle recovery following exercise: A systematic review and meta-analysis. International Journal of Sport Nutrition and Exercise Metabolism, 34(6), 378–392.
https://journals.humankinetics.com/view/journals/ijsnem/34/6/article-p378.xml